How to Talk to Someone Who Is Dying
It’s so human, to worry about getting this wrong.
Saying something careless.
Making it worse.
Worry that bringing up death will somehow make it more real.
So we stay quiet.
Or overcompensate with forced optimism.
Or avoid visiting altogether.
If someone you love is dying, you might carrying a quiet question:
What do I say?
The truth is, there isn’t a perfect script.
But there are ways of approaching the conversation that feel steadier — and more human.
When someone we love is approaching the end of life, we’re suddenly aware of how little control we have. That awareness can show up as anxiety, silence, or forced positivity.
Why This Conversation Feels So Hard
Talking to someone who is dying confronts us with our own limits.
We can’t fix it, reverse it, or control the outcome.
In a culture that values solutions and productivity, sitting in a room where nothing can be “fixed” feels destabilizing. It’s why so many avoid the topic all together.
There is also fear of:
Making them more afraid
Saying the wrong thing
Breaking down emotionally
Seeing their physical decline
Being confronted with our own mortality
Sometimes we avoid the conversation because we care deeply.
We don’t want to make them more afraid.
We don’t want to cry too much.
We don’t want to freeze.
We don’t want to regret the conversation later.
But silence can unintentionally communicate distance.
What most people who are dying need is not perfection.
I’ve sat in rooms where people (including me) weren’t sure what to say, and I’ve learned that just being there, present and yourself, matters more than perfectly chosen words.
What Matters More Than Saying the Right Thing
If you remember nothing else from this post, remember this:
There are no perfect words, so you can’t choose wrong.
You do need to be regulated enough to stay.
Presence matters more than perfection.
You can sit beside someone and say very little — and still communicate care.
Often, what makes conversations feel supportive is:
Eye contact
Gentle tone
Willingness to listen
Not rushing the moment
Letting silence exist
Sometimes silence is respect.
Simple Things You Can Say
If you’re wondering what to say to someone who is dying, here are phrases that honor what’s happening without forcing or pretending you know what to say.
“I didn’t know what to say, but I wanted to be here.”
“I’ve been thinking about you.”
“This is hard. I’m really glad I get to sit with you.”
“You don’t have to carry this alone.”
“If there’s something you want to talk about, I’m here.”
“We don’t have to make this a big conversation. I just wanted to see you.”
“I’m not going anywhere.”
“I care about you. That’s really it.”
“If today feels quiet, that’s okay too.”
“I don’t have the right words — but I’m here.”
And if the moment calls for something slightly more direct:
“I know things are changing.”
“If you want to talk about what’s ahead, I won’t avoid it.”
“What feels most real for you today?”
Notice what these do:
They invite.
They don’t assume.
They allow choice.
When someone is dying, so much is out of their control.
Connection that restores even small autonomy matters.
What Not to Say (And Why)
There are certain phrases people reach for out of discomfort.
Not because they’re unkind — but because they don’t know what else to say and these are somewhat common if you grow up in the US.
Avoid:
“Everything happens for a reason.”
“Stay positive.”
“God’s got a plan” (unless you know explicitly that this person has this belief)
“You’re going to beat this.”
“At least you lived a long life.”
“It will all work out.”
These phrases shift the conversation away from the person’s lived reality, they can minimize fear, grief, or complexity.
Instead of reassuring, they can make someone feel unseen. You don’t need to be there to brighten the moment, you need to meet it.
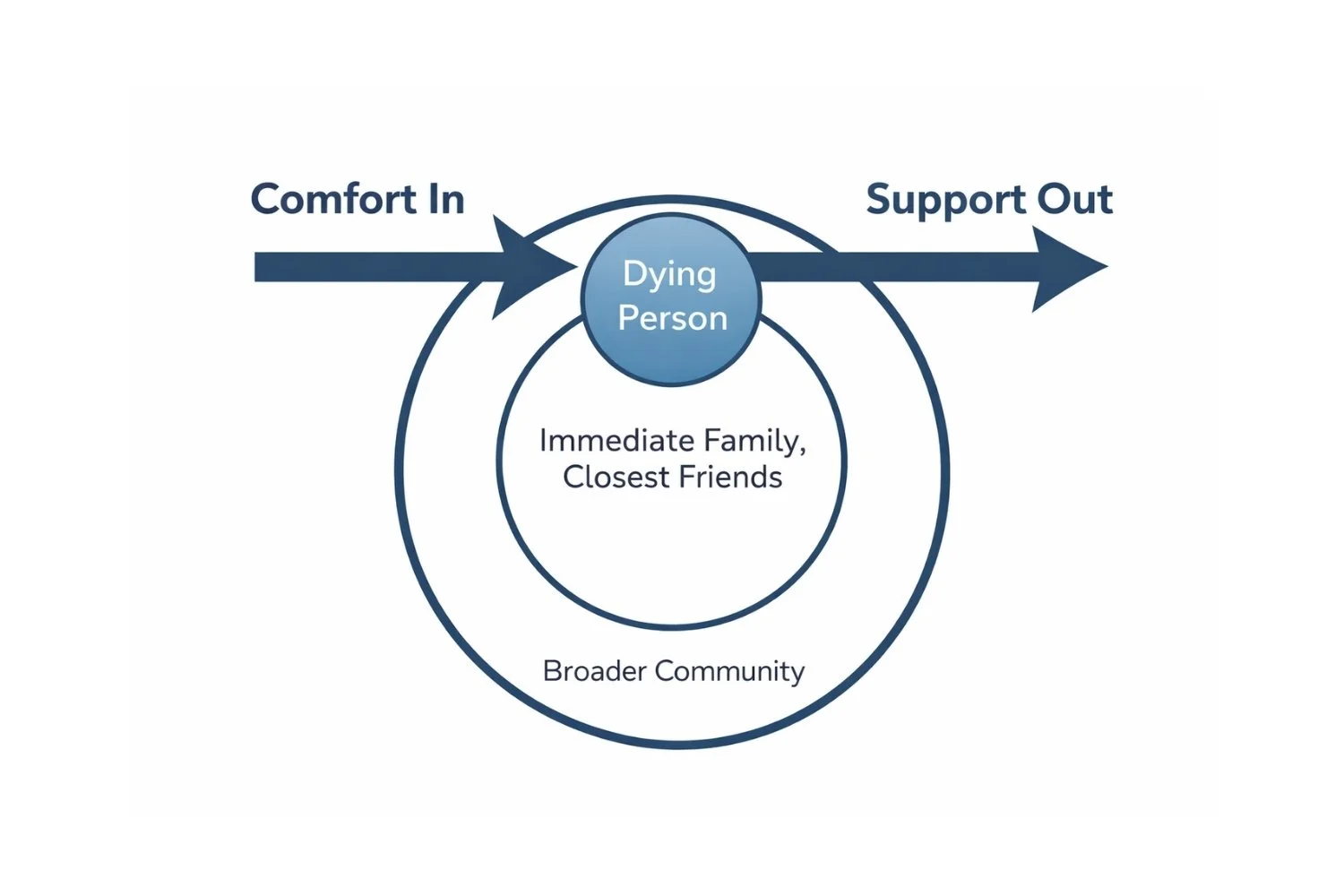
A Framework That Helps: Comfort In, Support Out
When someone is dying, emotions ripple outward through everyone who loves them. It can help to picture this as a series of circles.
The person who is dying is at the center.
Around them are the chosen people closest — a partner, children, siblings.
Beyond that are extended family, friends, coworkers, community.
Each circle matters. But the direction of emotional support matters too.
Support moves inward. Distress moves outward.
The person at the center shouldn’t have to manage anyone else’s fear. They’re already carrying enough.
If you’re in an outer circle, your role is to bring steadiness toward the center — and to take your own overwhelm somewhere further out.
That might mean calling a friend after a visit, stepping outside to cry, talking to a sibling who isn’t at the bedside, seeing a therapist, or finding a space where you can say honestly, “I’m not okay.”
Those feelings are real. They’re valid. They just shouldn’t be put on the dying person.
What often happens in end-of-life conversations is that people, understandably, panic. They’re hurting and scared.
They look at the person who is dying and say, “I don’t know how I’m going to survive this,” or “I can’t handle watching you like this.” And while those statements may be true, they place the emotional weight back onto the person who is already facing the most.
Loving someone at the end of life sometimes means holding your fear well enough that they don’t have to carry it for you.
It’s being thoughtful about where you put them.
When you process outward and bring steadiness inward, conversations soften. The room feels less chaotic. The person at the center can speak without also having to reassure everyone else.
It’s a simple framework. But it protects two important things:
The dignity of the person who is dying
The integrity of your relationship
When They Want to Talk About Death
Sometimes the person who is dying will bring it up directly.
They may say:
“I don’t think I have much time.”
“I’m scared.”
“What do you think happens?”
“I don’t want to suffer.”
Your instinct might be to soften or redirect. Instead, try staying with it.
You can respond with:
“What feels most frightening about it?”
“Do you want to talk more about that?”
“I’m listening.”
“Tell me more.”
You don’t need answers, presence is enough. Don’t fill the silence with words.
Let them define the depth of the conversation.
Some days they may want to talk openly about dying. Other days they may want to talk about TV, TikTok, sports, or nothing at all.
Follow their lead.
If They Don’t Want to Talk About It
Not everyone wants explicit conversations about death, and that’s okay.
Support can look like:
Sharing stories
Looking at old photos
Watching comforting shows
Sitting quietly
Talking about everyday life
Connection does not always require heavy topics. Let the person set the emotional temperature, and don’t be afraid to ask.
A Personal Reflection
When my brother was in hospice at our home, I remember sitting beside him, so completely unsure of what I was supposed to say.
I kept thinking there must be something I should offer — something profound, something that would matter later.
Now, I don’t even remember waht I said, I just remember being there. The love.
I learned that being present — even awkwardly, especially imperfectly — mattered more than finding the right words.
That experience changed how I think about these conversations.
If the Relationship Is Complicated
Not every relationship at end-of-life is simple.
There may be:
Estrangement
Unresolved tension
Old injuries
Mixed feelings
You shouldn’t have to force emotional closure. You don’t have to force forgiveness.
You can say:
“I’m glad I’m here.”
“I care about you.”
“I wanted to see you.”
That may be enough. Complicated relationships often hold grief layered with ambivalence.
That doesn’t make you cold, you’re human.
Practical Considerations When Talking to Someone in Hospice
If your loved one is in hospice or nearing the end of life, practical awareness helps.
Energy levels fluctuate, attention shortens. Physical discomfort can limit conversation.
Keep visits:
Shorter rather than longer
Flexible
Attuned to fatigue
Grounded in the present
Sometimes the most supportive thing is to:
Adjust a pillow
Offer water
Sit quietly
Step out when they need rest
Talking is not the only form of connection.
When You Feel Overwhelmed
You may notice your own emotions rising:
Grief
Fear
Anticipation
Helplessness
It’s important to separate your emotional processing from theirs.
If you need to cry, step out and cry. If you need to talk about your fear, speak to a friend or therapist.
Don’t rely on the dying person to regulate you.
That doesn’t mean you suppress your feelings, it just means you choose where to express them.
The Role of Listening
Listening at end-of-life is different from listening in everyday life.
You’re not listening to respond, but to witness.
If they:
Repeat stories
Express regret
Exagerate/spin
Revisit memories
Voice fear
Stay with it.
Repetition is often part of emotional integration.
You can say:
“That sounds important.”
“Tell me more.”
“What a vivid/funny/amazing/insane moment!”
“I’m glad you’re sharing that.”
When Words Fail
Language will feel inadequate sometimes. For those moments, you use your loving presence.
Hold their hand.
Sit beside them.
Breathe slowly.
Human presence predates language, it’s often enough. We knew how to seek and give comfort before we knew how to talk.
Don’t Try To Be Perfect
If you’re searching for how to talk to someone who is dying, you probably care deeply. That matters the most.
You may:
Say something imperfect.
Cry unexpectedly.
Freeze for a moment.
The goal is not to get the words exactly right, we’re just trying to stay connected.
A Final Thought
When someone you love is dying, conversation becomes less about information and more about relationship.
You can’t be there to try to solve death.
Stay curious.
Stay honest.
Stay.
That is what will be remembered.